What Causes Trigger Points?
From Desk Work to Deadlifts: The Science of Why Muscles Develop Painful Knots
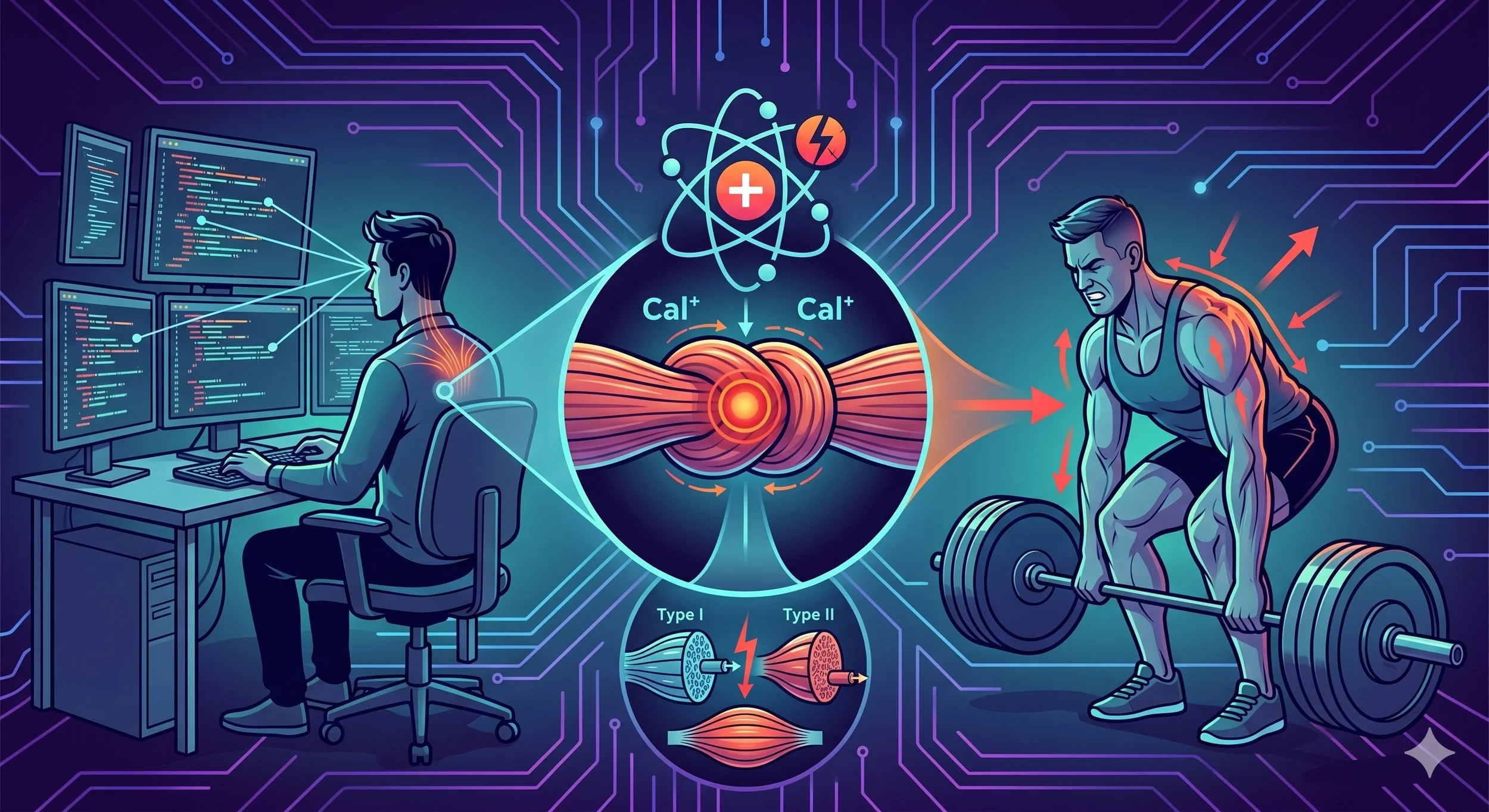
A software developer who sits all day and a competitive athlete who trains six days a week can both develop the same painful trigger points. The mechanisms behind each are different, but they converge on a shared metabolic problem. Here is what the research tells us about why trigger points form, which muscle fibers are most vulnerable, and why there is still scientific disagreement about the fundamental cause.
- Trigger points can develop from at least six distinct types of muscle overload, ranging from sustained low-force postures to maximal athletic efforts (Bron & Dommerholt, 2012).
- The "Cinderella Hypothesis" explains a counterintuitive finding: the lightest tasks may damage certain motor units precisely because those fibers never get a break (Hagg, 1991).
- In one controlled study, trigger point sensitivity increased in the upper trapezius during computer work, with visual demand (not posture) as the primary factor (Treaster et al., 2006).
- Calcium dysregulation appears to be a common thread across overload types. Even low-frequency muscle stimulation can triple intracellular calcium concentrations, driving sustained contraction and membrane damage (Gissel, 2000).
- Non-mechanical factors also matter: emotional stress may activate trigger points through sympathetic pathways, and internal organ pathology can sensitize muscles through viscerosomatic reflexes.
- The integrated trigger point hypothesis is the most widely accepted model, but six alternative hypotheses challenge or extend it, and no single theory has been definitively proven.
Are Muscle Overload or Repetitive Strain Causing Your Pain?
Whether your trigger points developed from desk work, athletic training, or chronic stress, our practitioners specialize in identifying the root cause and treating it directly with dry needling and targeted manual therapy.
Schedule NowThe Paradox: Why Light Tasks Can Hurt as Much as Heavy Ones
If trigger points were simply a product of "working too hard," we would expect them primarily in athletes and manual laborers. Instead, some of the most stubborn trigger points show up in people who sit at desks, play violin, or perform dental work. The force demands on their muscles are minimal. So why does the tissue break down?
The answer begins with how the nervous system selects which muscle fibers to use. In the 1960s, Henneman and colleagues established what became known as the Size Principle: when a muscle contracts, motor units are activated in order from smallest to largest. Small, slow-twitch motor units handle low-force tasks. Larger, fast-twitch units are only called upon when more force is needed (Henneman et al., 1965).
This means that during a light task like holding your head upright or resting your fingers on a keyboard, only a small population of Type I motor units is engaged. These fibers handle the entire workload. And because the task demands little overall force, the nervous system sees no reason to rotate in fresh motor units.
Goran Hagg recognized the clinical significance of this pattern and proposed what he called the "Cinderella Hypothesis." Named for the fairy tale character who is the first to start working and the last to stop, these low-threshold motor units bear a metabolic burden out of proportion to the force they produce. Over hours of sustained activation, they exhaust their energy reserves while the vast majority of the muscle sits idle (Hagg, 1991).
This hypothesis has been supported by electromyographic research showing that specific motor units in the trapezius remain continuously active during prolonged computer work, even as overall muscle activation levels rise and fall. The "Cinderella" fibers never rotate out.
Related What Is Myofascial Pain? The Integrated Hypothesis ExplainedWhat One Hour of Typing Does to Your Trapezius
Treaster and colleagues tested the Cinderella Hypothesis directly by monitoring trigger point development in 16 female subjects during computer work. The study varied both postural conditions (high and low stress) and visual conditions (high and low stress) to isolate which factors mattered most (Treaster et al., 2006).
The results challenged conventional thinking. Only the conditions involving high visual stress (small font, low contrast) produced a statistically significant increase in trigger point sensitivity, as assessed by both expert palpation and subject self-report. Higher postural stress alone did not produce the same effect. This finding suggests that the cognitive and visual demands of screen work may drive upper trapezius tension through central nervous system pathways, not just through the mechanical load on the neck and shoulders.
This has direct implications for how we think about workplace ergonomics. An endodontist with nearly ideal workstation setup (shoulders relaxed, forearms supported, wrists in slight extension) can still develop severe neck and shoulder pain because the problem is not fundamentally about posture. It is about the sustained metabolic cost imposed on a small subset of muscle fibers by continuous low-level activation, amplified by the demands of visual concentration (Franssen et al., 2011).
Calcium: The Molecule That Locks Muscles in Contraction
Regardless of whether the overload comes from desk work, running, or lifting, the downstream problem converges on the same molecule: calcium. Calcium ions are the signal that initiates muscle contraction. When calcium floods the space around muscle filaments, it allows myosin to bind to actin and the fiber shortens. Normally, calcium is rapidly pumped back into storage (the sarcoplasmic reticulum) after each contraction. But when this system fails, the muscle fiber stays contracted.
Gissel's research demonstrated that even low-frequency, low-intensity electrical stimulation of skeletal muscle (1 Hz for 240 minutes, simulating prolonged light activity) can increase calcium uptake dramatically: by 30% in slow-twitch soleus muscle and by 154% in fast-twitch extensor digitorum longus. Free intracellular calcium concentrations rose as much as threefold. The study also showed that this calcium overload triggered leakage of intracellular enzymes through the cell membrane, suggesting structural damage to the muscle fiber itself (Gissel, 2000).
This finding is significant because it demonstrates that prolonged low-level muscle activity, not just intense exercise, can produce the kind of calcium dysregulation that would sustain a trigger point contraction. Gissel specifically proposed that calcium plays a central role in muscle fiber injury during the kind of prolonged activity experienced by computer mouse users.
A separate line of research showed that mitochondrial calcium leakage can produce chronically elevated cytosolic calcium, leading to disruption of calcium-dependent proteins, cell death, and tissue remodeling (Sirvent et al., 2005). This pathway may explain why some trigger points persist for months or years: the mitochondria themselves become damaged, creating a steady leak of calcium that sustains the contraction cycle even without ongoing external overload.
| Pathway | What Goes Wrong | Why It Matters |
|---|---|---|
| Low-frequency stimulation overload | Prolonged light activity increases calcium influx and overwhelms the cell's ability to pump it back into storage | Explains how desk work and light repetitive tasks produce tissue damage over time |
| Mitochondrial leak | Damaged mitochondria continuously release stored calcium into the cell | May explain why chronic trigger points persist long after the original overload is removed |
| Sarcoplasmic reticulum disruption | Mechanical damage (especially from eccentric loading) tears the membrane that stores calcium | Explains the overlap between delayed-onset muscle soreness and trigger point formation after exercise |
What Overloaded Muscle Looks Like Under a Microscope
Hagg reviewed ten biopsy studies examining muscle fiber abnormalities in workers exposed to occupational loading. The review focused primarily on the upper trapezius, with additional data from hand and forearm muscles. The key findings in subjects with myalgia or occupational exposure included enlarged fiber cross-sectional areas, multiple indicators of mitochondrial disturbance in Type I fibers, and reduced capillarization relative to fiber size in women (Hagg, 2000).
Two specific fiber abnormalities were identified. "Ragged red" fibers indicate structural breakdown of the cell membrane and mitochondria. "Moth-eaten" fibers show disrupted distribution of mitochondria or the sarcotubular system, a pattern consistent with chronic oxygen deprivation. Both findings align with the ischemia and energy crisis model described in the integrated trigger point hypothesis.
Hagg noted an important caveat: some signs of mitochondrial disturbance were also found in reference groups, and the relationship between these findings and pain perception remains unclear. However, there were indications that the degree of fiber abnormality correlated with the severity of pain, supporting the idea that these structural changes are clinically meaningful rather than incidental.
Chronic Pain That Keeps Coming Back Despite Stretching?
If your trigger points return despite stretching, foam rolling, and ergonomic adjustments, the underlying cause may involve metabolic overload of specific motor units or calcium dysregulation. Dry needling targets the source directly.
Schedule NowThe Athlete's Version: How Exercise Creates Trigger Points
While the Cinderella pathway dominates in sedentary and occupational populations, athletes encounter trigger points through different mechanisms. Understanding these pathways helps explain why training-related trigger points often behave differently from desk-work trigger points and may respond to different treatment approaches.
Eccentric Loading and Cytoskeletal Damage
There is no definitive proof that eccentric contractions directly cause trigger points, but the overlap between eccentric muscle damage and trigger point pathophysiology is extensive (Bron & Dommerholt, 2012). During eccentric work (muscle lengthening under load), fast-twitch fibers that cannot regenerate ATP quickly enough enter a state of high stiffness. When stiffer fibers are then stretched further by the ongoing movement, the mechanical force disrupts internal structural proteins, particularly desmin (which links adjacent myofibrils together) and titin (which provides elastic recoil). Researchers have observed that fibers in eccentrically exercised muscles can swell to approximately four times their normal cross-sectional area.
Eccentric loading also damages the sarcoplasmic reticulum, releasing calcium stores directly into the cell interior. As described above, this elevated calcium keeps actin and myosin locked together and can damage the cell membrane further, creating a self-reinforcing cycle of contraction, damage, and more contraction.
When ATP Runs Out
During high-intensity concentric work, the muscle draws on stored ATP for the first few seconds, then shifts to creatine phosphate (CP) to regenerate ATP. This combined system sustains maximal output for roughly 14 to 16 seconds. After that window closes, the cell increasingly depends on anaerobic glycolysis, which produces ATP more slowly and generates acidic byproducts that lower local pH (Bron & Dommerholt, 2012).
If the work continues long enough to fully deplete local ATP stores, a critical threshold is crossed. ATP is not only the fuel for contraction; it is also required for the "release" step. Without ATP, the myosin head cannot detach from actin. The result is a rigid, locked sarcomere. This is the same biochemical mechanism behind rigor mortis, and it may represent the initiating event for trigger point formation during intense training sessions that push beyond the muscle's metabolic capacity.
Related Active vs. Latent Trigger Points: Types, Differences, and TreatmentWhen the Cause Is Not Mechanical: Stress and Visceral Pain
Not all trigger points originate from physical overload. Two non-mechanical pathways are well-documented: psychological stress and visceral referral (Gerwin et al., 2004).
Emotional Stress and Sympathetic Activation
Banks and colleagues showed that autogenic relaxation training could reduce the electrical activity recorded at active trigger point sites, demonstrating a measurable link between psychological state and trigger point behavior (Banks et al., 1998). The proposed mechanism runs through the sympathetic nervous system: emotional stress increases sympathetic output, which in turn may stimulate acetylcholine release at the motor endplate through adrenergic receptor activation. This means that anxiety, work pressure, or emotional trauma can directly amplify the contraction cycle that maintains trigger points, even in the absence of any physical overload on the muscle.
Visceral Referral Patterns
Internal organ pathology can also drive trigger point formation in the muscles that share segmental innervation with the affected organ. Giamberardino and colleagues described two distinct patterns: referred pain from viscera that occurs without increased tissue sensitivity, and referred pain accompanied by hyperalgesia in the muscle layer, often involving palpable trigger points that may extend into the subcutaneous tissue and skin (Giamberardino et al., 1999). This explains why patients with conditions such as endometriosis, kidney stones, or inflammatory bowel disease frequently develop concurrent myofascial pain in the abdominal wall, flank, or pelvic floor. Treating the trigger points without addressing the visceral source typically provides only temporary relief.
Related Acupuncture for Myofascial Pain SyndromeThe Scientific Debate: Six Alternative Theories
The integrated trigger point hypothesis, which frames trigger points as a local motor endplate disorder sustained by an energy crisis, is the most cited model in the literature. But it is far from settled science. At least six alternative hypotheses propose fundamentally different mechanisms. Some complement the integrated model; others directly challenge it.
| Hypothesis | Key Proponent | Central Claim | Strength | Limitation |
|---|---|---|---|---|
| Neuritis | Quintner, Bove & Cohen (2014) | Trigger points are not primary muscle lesions at all. Focal inflammation of peripheral nerves creates ectopic sensitivity and spontaneous nociceptor firing. The palpable nodule is a site of secondary allodynia driven by altered central processing. | Provides a plausible neurophysiological alternative grounded in known nerve biology. The most methodologically rigorous critique of the TrP concept. | Proposes that TrPs as pathological entities lack scientific basis, a position most clinicians find difficult to reconcile with daily clinical findings. |
| Central Modulation | Hocking (2010, 2013) | Trigger points arise from sustained alpha-motoneuron plateau depolarizations maintained by the central nervous system. These plateau potentials can persist for seconds after the original excitatory input has stopped. | Explains how trigger points could be maintained by central rather than peripheral mechanisms. Distinguishes "antecedent" TrPs (from nociceptive withdrawal reflexes) from "consequent" TrPs (from compensatory motor facilitation). | Requires further experimental validation. The proposed research projects to test the hypothesis have not yet been completed. |
| Radiculopathy (IMS) | Gunn | The nerve root is the primary site of pathology. Impaired nerve flow makes innervated structures (especially striated muscle) atrophic, irritable, and supersensitive. Trigger points are one clinical manifestation of this broader radiculoneuropathic pattern. | Aligns with the clinical observation that trigger points often follow dermatomal and myotomal patterns, and that spinal pathology frequently coexists with myofascial pain. | Relies heavily on Cannon and Rosenblueth's "Law of Denervation," which some researchers consider an oversimplification of nerve-muscle interaction. |
| Neurogenic | Srbely (2010) | Trigger points are secondary neurogenic phenomena arising from primary pathologies within the same spinal segment. Central sensitization, not local endplate dysfunction, is the root cause. | Supported by the observation that inactivating trigger points can reduce central sensitization. | Evidence base is limited primarily to Srbely's own studies; independent replication is needed. |
| Mechanistic (X-ROS) | Jafri (2014) | Mechanical stretching of muscle activates a mechano-sensitive enzyme (NOX2) that generates stretch-activated reactive oxygen species (X-ROS). Pathologic increases in X-ROS production destabilize calcium signaling and may serve as a disease modifier for trigger point formation. | Introduces a novel molecular pathway (oxidative stress via NADPH oxidase) that bridges mechanical loading with calcium dysregulation at the subcellular level. | Largely theoretical; direct experimental confirmation in the context of myofascial trigger points is still needed. |
| Neurophysiologic | Partanen (1999, 2010) | The spontaneous electrical activity recorded at trigger points originates from intrafusal muscle spindle fibers, not from extrafusal motor endplates. Taut bands result from spindle inflammation and gamma/beta efferent activation. | Raises important questions about the assumed source of endplate noise. | No convincing evidence has been presented that endplate noise originates in intrafusal fibers (Wiederholt, 1970). |
The practical takeaway from this ongoing scientific debate is not that we should discard the integrated hypothesis, but that trigger points probably involve more than just local endplate dysfunction. Peripheral mechanisms (metabolic crisis, calcium dysregulation, mechanical damage) and central mechanisms (sensitization, plateau potentials, autonomic amplification) likely interact in ways that vary from patient to patient. Clinicians who can recognize which mechanisms are dominant in a given case are better positioned to select the most effective treatment approach.
Why It Matters for Your Treatment
The cause of your trigger points shapes what will actually resolve them. An office worker whose pain stems from Cinderella motor unit fatigue may benefit more from microbreak strategies and targeted dry needling of overloaded fibers than from postural correction alone. An athlete whose trigger points developed after eccentric loading needs a recovery protocol that addresses calcium overload and cytoskeletal repair, not just foam rolling. A patient whose trigger points flare with anxiety or during menstrual cycles may need treatment that incorporates the autonomic and visceral contributions alongside the local muscle work.
In all cases, addressing the trigger point directly (through dry needling, for example) is often the most efficient starting point because it disrupts the self-sustaining contraction cycle regardless of which pathway initiated it. But lasting results typically require also addressing the upstream cause: the work pattern, the training load, the stress response, or the visceral condition that set the process in motion.
Related Trigger Points Guide: Complete Muscle Index and Treatment Overview Next in Series Part 3: Why Does Muscle Pain Spread? Peripheral Sensitization and Referred Pain Continue Reading Part 4: Why Chronic Pain Gets Worse Over TimeExpert Trigger Point Diagnosis and Treatment at Morningside Acupuncture
At Morningside Acupuncture, we are the highest-rated acupuncture and dry needling clinic in New York City with over 500 five-star Google reviews. Our practitioners identify the specific type of muscle overload driving your trigger points and design treatment plans that address the cause, not just the symptoms. Whether your pain comes from desk work, training, stress, or a combination of factors, we can help.
Schedule NowReferences
- Banks, S.L., Jacobs, D.W., Gevirtz, R., & Hubbard, D.R. (1998). Effects of autogenic relaxation training on electromyographic activity in active myofascial trigger points. Journal of Musculoskeletal Pain, 6(4), 23-32.
- Bron, C., & Dommerholt, J. (2012). Etiology of myofascial trigger points. Current Pain and Headache Reports, 16(5), 439-444. https://doi.org/10.1007/s11916-012-0289-4
- Franssen, J., Bron, C., & Dommerholt, J. (2011). Myofascial trigger points in the workplace. In C. Fernandez-de-las-Penas, J.A. Cleland, & P. Huijbregts (Eds.), Neck and Arm Pain Syndromes: Evidence-Informed Screening, Diagnosis, and Management (pp. 78-93). Edinburgh: Elsevier.
- Gerwin, R.D., Dommerholt, J., & Shah, J.P. (2004). An expansion of Simons' integrated hypothesis of trigger point formation. Current Pain and Headache Reports, 8(6), 468-475. https://doi.org/10.1007/s11916-004-0069-x
- Giamberardino, M.A., Affaitati, G., Iezzi, S., et al. (1999). Referred muscle pain and hyperalgesia from viscera. Journal of Musculoskeletal Pain, 7(1/2), 61-69. https://doi.org/10.1300/J094v07n01_07
- Gissel, H. (2000). Ca2+ accumulation and cell damage in skeletal muscle during low frequency stimulation. European Journal of Applied Physiology, 83(2-3), 175-180. https://doi.org/10.1007/s004210000276
- Hagg, G.M. (1991). Static work and myalgia: A new explanation model. In P.A. Andersson, D.J. Hobart, & J.V. Danoff (Eds.), Electromyographical Kinesiology (pp. 115-199). Amsterdam: Elsevier.
- Hagg, G.M. (2000). Human muscle fibre abnormalities related to occupational load. European Journal of Applied Physiology, 83(2-3), 159-165. https://doi.org/10.1007/s004210000274
- Henneman, E., Somjen, G., & Carpenter, D.O. (1965). Excitability and inhibitability of motoneurons of different sizes. Journal of Neurophysiology, 28(3), 599-620. https://doi.org/10.1152/jn.1965.28.3.599
- Hocking, M.J.L. (2010). Trigger points and central modulation: A new hypothesis. Journal of Musculoskeletal Pain, 18(2), 186-203. https://doi.org/10.3109/10582452.2010.483965
- Hocking, M.J. (2013). Exploring the central modulation hypothesis: Do ancient memory mechanisms underlie the pathophysiology of trigger points? Current Pain and Headache Reports, 17, 347. https://doi.org/10.1007/s11916-013-0347-6
- Hubbard, D.R. (1996). Chronic and recurrent muscle pain: Pathophysiology and treatment, and review of pharmacologic studies. Journal of Musculoskeletal Pain, 4(1-2), 123-143. https://doi.org/10.1300/J094v04n01_08
- Jafri, M.S. (2014). Mechanisms of myofascial pain. International Scholarly Research Notices, 2014, 523924. https://doi.org/10.1155/2014/523924
- Quintner, J.L., Bove, G.M., & Cohen, M.L. (2014). A critical evaluation of the trigger point phenomenon. Rheumatology, 54(3), 392-399. https://doi.org/10.1093/rheumatology/keu471
- Sirvent, P., Mercier, J., Vassort, G., & Lacampagne, A. (2005). New insights into mechanisms of statin-associated myotoxicity. Biochemical and Biophysical Research Communications, 338(3), 1426-1434.
- Srbely, J.Z. (2010). New trends in the treatment and management of myofascial pain syndrome. Current Pain and Headache Reports, 14(5), 346-352. https://doi.org/10.1007/s11916-010-0128-4
- Treaster, D., Marras, W.S., Burr, D., Sheedy, J.E., & Hart, D. (2006). Myofascial trigger point development from visual and postural stressors during computer work. Journal of Electromyography and Kinesiology, 16(2), 115-124. https://doi.org/10.1016/j.jelekin.2005.06.016
- Visser, B., & van Dieen, J.H. (2006). Pathophysiology of upper extremity muscle disorders. Journal of Electromyography and Kinesiology, 16(1), 1-16. https://doi.org/10.1016/j.jelekin.2005.06.005
Disclaimer: This web site is intended for educational and informational purposes only. Reading this website does not constitute providing medical advice or any professional services. This information should not be used for diagnosing or treating any health issue or disease. Those seeking medical advice should consult with a licensed physician. Seek the advice of a medical doctor or other qualified health professional for any medical condition. If you think you have a medical emergency, call 911 or go to the emergency room. No acupuncturist-patient relationship is created by reading this website or using the information. Morningside Acupuncture PLLC and its employees and contributors do not make any express or implied representations with respect to the information on this site or its use. For any legal interpretation of scope of practice in your state, consult a licensed attorney or regulatory authority.